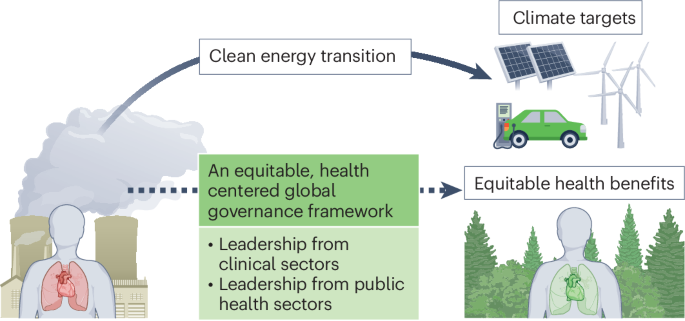
Integrating health equity into energy transitions and climate governance
Key Takeaway:
Integrating health equity into climate policies is crucial to ensure everyone benefits equally from cleaner energy, preventing health disparities as we transition to sustainable practices.
For Clinicians:
"Qualitative study. No sample size. Highlights potential health disparities in energy transitions. Lacks quantitative data. Consider health equity in climate-related policies. Await further research for clinical implications."
For Everyone Else:
This research is in early stages. It highlights potential health benefits from clean energy policies. It may take years to impact care. Continue following your doctor's advice for your health needs.
Citation:
Nature Medicine - AI Section, 2026. DOI: s41591-026-04290-0 Read article →
